ACLS Provider Manual PDF: A Comprehensive Guide (2026)
Essential for certification, the 2026 ACLS provider manual PDF offers a detailed study guide covering algorithms, pharmacology, and BLS integration for advanced care.
Advanced Cardiovascular Life Support (ACLS) represents the highest level of resuscitation training, focusing on complex cardiovascular emergencies. The ACLS Provider Manual PDF serves as the cornerstone resource for healthcare professionals seeking certification or recertification. This comprehensive guide, updated for 2026, details systematic approaches to managing cardiac arrest, bradycardia, and tachycardia, ensuring consistent, evidence-based care.
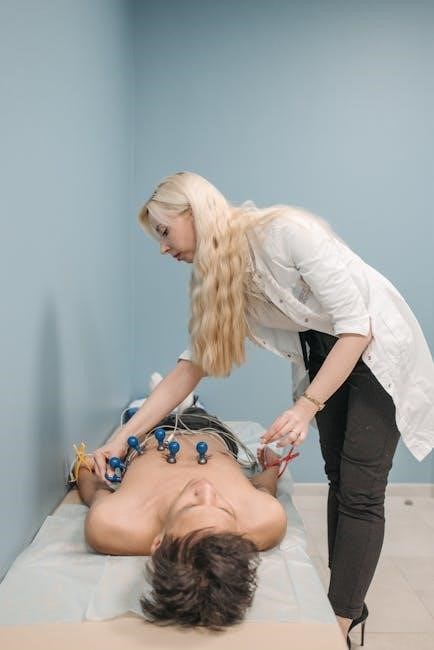
The manual isn’t merely a reference; it’s a structured learning tool. It outlines the crucial ABCD approach – Airway, Breathing, Circulation, and Drugs – providing a framework for rapid assessment and intervention. It integrates Basic Life Support (BLS) principles, recognizing that effective foundational skills are paramount. Furthermore, the manual details essential pharmacological interventions, including dosage guidelines and considerations for potential drug interactions.
Access to the official PDF is vital, as it reflects the latest American Heart Association (AHA) guidelines. Understanding the content within prepares providers for both the written exam and practical skills assessments, ultimately enhancing patient outcomes during critical events. Regular updates and continuing education are key to maintaining proficiency.
Importance of the ACLS Provider Manual PDF
The ACLS Provider Manual PDF is paramount for several reasons. Firstly, it ensures standardized care, aligning all providers with the latest American Heart Association (AHA) guidelines. This consistency is critical during high-stress, time-sensitive emergencies. Secondly, the manual functions as a vital study aid, preparing healthcare professionals for the rigorous ACLS certification process, encompassing both written and practical evaluations.
Having the PDF allows for convenient, on-demand access to crucial information regarding resuscitation algorithms, pharmacological interventions, and airway management techniques. It’s a portable resource for quick reference in clinical settings and facilitates continuous learning. The manual’s detailed explanations of the ABCD approach and BLS integration reinforce fundamental skills.
Furthermore, the PDF format enables easy searching and note-taking, enhancing comprehension and retention. Staying current with the manual’s content is not just about certification; it’s about providing the highest quality of care and improving patient survival rates in critical cardiovascular events.
Where to Find the Official ACLS Provider Manual PDF
The primary and most reliable source for the official ACLS Provider Manual PDF is the American Heart Association (AHA) website. Access is typically granted upon enrollment in an AHA ACLS course. Purchasing the manual directly from the AHA guarantees you receive the most up-to-date version, reflecting the latest guidelines and protocols.
Authorized AHA training centers also provide the manual, either as a physical copy or through digital access codes linked to the PDF. Be cautious of unofficial sources offering free downloads, as these may contain outdated information or be of questionable legality.
Reputable online medical bookstores sometimes carry the official PDF, but always verify the source’s accreditation. Avoid websites promising “free” PDFs without proper authorization. Ensuring you have the official AHA manual is crucial for accurate training and adherence to established advanced life support standards, safeguarding both provider competence and patient safety.

Understanding ACLS Core Concepts
ACLS builds upon BLS, emphasizing the ABCD approach – airway, breathing, circulation, and drugs – for effective advanced cardiac care interventions.
The ABCD Approach to ACLS
Airway assessment and management are paramount, ensuring a patent airway for effective ventilation. This includes techniques like head-tilt/chin-lift and adjuncts if needed. Breathing evaluation focuses on respiratory rate, depth, and oxygen saturation, requiring interventions like assisted ventilation if compromised.
Circulation assessment involves pulse checks, blood pressure monitoring, and identifying perfusion deficits. Early recognition of shock states is crucial, guiding fluid resuscitation and vasopressor support. Finally, Drugs play a vital role, with ACLS protocols dictating specific medications and dosages for cardiac arrest, bradycardia, and tachycardia.
This systematic approach, detailed within the ACLS provider manual, ensures a structured response to cardiovascular emergencies. Prioritizing these elements allows healthcare professionals to rapidly identify and address life-threatening conditions, improving patient outcomes. Consistent application of the ABCD framework is fundamental to successful ACLS resuscitation efforts.
Basic Life Support (BLS) Review within ACLS
ACLS builds upon a solid foundation of BLS skills. The provider manual emphasizes high-quality CPR, including appropriate compression rate, depth, and minimal interruptions. Effective chest compressions are vital for maintaining cerebral and myocardial perfusion until advanced interventions can be initiated.
Ventilation with a bag-valve mask (BVM) is also reviewed, stressing adequate tidal volume and avoiding hyperventilation. Recognizing the importance of early defibrillation, the manual details proper AED usage and integration into the resuscitation sequence. Team dynamics and clear communication during CPR are highlighted as critical components.
The ACLS course reinforces these BLS principles, ensuring providers can seamlessly transition from basic to advanced life support. Proficiency in BLS is not merely a prerequisite, but a continuously practiced skill throughout the ACLS algorithm implementation, directly impacting patient survival rates.
Airway Management Techniques in ACLS
Secure airway management is paramount in ACLS. The provider manual details techniques ranging from simple adjuncts like oropharyngeal and nasopharyngeal airways to advanced methods like endotracheal intubation. Proper preparation, including equipment checks and suction availability, is emphasized.
Rapid sequence intubation (RSI) is covered, outlining medication dosages and potential complications. Alternative airway strategies, such as supraglottic airways (SGAs), are presented as valuable tools when intubation is challenging or unsuccessful. Continuous capnography monitoring is crucial to confirm correct endotracheal tube placement.
The manual stresses the importance of recognizing and managing airway obstruction, including foreign body removal. Maintaining oxygenation and ventilation throughout the process is critical. Post-intubation care, including cuff pressure management and sedation, is also addressed, ensuring optimal patient outcomes during resuscitation efforts.

Advanced Cardiovascular Life Support Algorithms
ACLS algorithms, detailed in the provider manual PDF, systematically guide healthcare professionals through managing cardiac arrest, bradycardia, and tachycardia scenarios.
ACLS Algorithm for Cardiac Arrest
The ACLS cardiac arrest algorithm, comprehensively outlined within the provider manual PDF, prioritizes immediate high-quality CPR. Initial steps involve confirming arrest and activating emergency response systems. Simultaneously, begin chest compressions at a rate of 100-120 per minute and a depth of at least 2 inches, minimizing interruptions.
Following compressions, the algorithm directs providers to assess the rhythm. For shockable rhythms – Ventricular Fibrillation (VF) and Pulseless Ventricular Tachycardia (pVT) – defibrillation is indicated. Non-shockable rhythms, Asystole and Pulseless Electrical Activity (PEA), require continued CPR and focus on identifying and treating reversible causes, often remembered using the “Hs and Ts” mnemonic (Hypovolemia, Hypoxia, Hydrogen ion, Hypo/Hyperkalemia, Hypothermia, Tension pneumothorax, Tamponade, Toxins, Thrombosis).
Epinephrine administration is crucial for both shockable and non-shockable rhythms, given every 3-5 minutes. The ACLS provider manual PDF emphasizes the importance of a coordinated team approach and continuous assessment throughout the resuscitation process, aiming for Return of Spontaneous Circulation (ROSC).
ACLS Algorithm for Bradycardia
The ACLS bradycardia algorithm, detailed in the provider manual PDF, systematically addresses symptomatic bradycardia – a heart rate below 60 bpm causing instability. Initial assessment focuses on the patient’s condition; is the bradycardia causing hypotension, altered mental status, or chest pain? If so, intervention is required.
The algorithm prioritizes atropine as the first-line medication, aiming to increase the heart rate. If atropine is ineffective, or unavailable, dopamine or epinephrine infusions are indicated. Transcutaneous pacing (TCP) serves as a rapid intervention for severe, symptomatic bradycardia, providing temporary electrical stimulation to the heart.

Underlying causes of bradycardia, such as medication effects or ischemia, must be identified and addressed. The ACLS provider manual PDF stresses continuous monitoring and reassessment, adjusting treatment based on the patient’s response. If the patient becomes unstable during treatment, prepare for potential escalation to advanced airway management and vasopressors.
ACLS Algorithm for Tachycardia
The ACLS tachycardia algorithm, comprehensively outlined in the provider manual PDF, differentiates between stable and unstable tachycardia. Initial assessment determines patient stability – presence of a pulse, blood pressure, altered mental status, or chest pain. Unstable patients require immediate synchronized cardioversion.
For narrow-complex tachycardias, vagal maneuvers are attempted first to slow the heart rate. If ineffective, adenosine is administered to interrupt AV nodal conduction. Wide-complex tachycardias are initially treated as ventricular tachycardia, with amiodarone or lidocaine as antiarrhythmic options.
The ACLS manual PDF emphasizes identifying and treating the underlying cause of tachycardia, such as electrolyte imbalances or ischemia. Continuous monitoring and reassessment are crucial, adjusting treatment based on the patient’s response. Prepare for potential escalation to defibrillation if the rhythm deteriorates to ventricular fibrillation.

Pharmacological Interventions in ACLS
ACLS relies on key drugs – epinephrine, amiodarone, adenosine – detailed in the provider manual PDF, with precise dosage guidelines for effective cardiac support.
Key ACLS Drugs and Their Administration
Essential ACLS pharmacological interventions center around several critical medications, meticulously outlined within the provider manual PDF. Epinephrine, a potent vasopressor, is fundamental in cardiac arrest, administered intravenously or intraosseously, typically in 1mg doses every 3-5 minutes.
Amiodarone, an antiarrhythmic, plays a crucial role in refractory ventricular fibrillation or pulseless ventricular tachycardia, given as a 150mg bolus followed by potential maintenance infusions. Adenosine is vital for stable supraventricular tachycardia, utilizing a rapid bolus followed by a saline flush.
Furthermore, the manual details the administration of vasopressin, often used as an alternative to epinephrine, and lidocaine for ventricular arrhythmias. Understanding proper dilution, administration techniques (IV push, infusion), and potential adverse effects – like hypotension or arrhythmias – is paramount. The ACLS provider manual PDF emphasizes the importance of timely and accurate drug delivery for optimal patient outcomes during critical cardiovascular events.
Dosage Guidelines for ACLS Medications
Precise medication dosages are critical in ACLS, comprehensively detailed within the provider manual PDF. Epinephrine for cardiac arrest mandates 1mg IV/IO every 3-5 minutes, with higher doses potentially considered under specific circumstances. Amiodarone, for refractory arrhythmias, begins with a 150mg IV bolus, potentially followed by a 1mg/minute infusion.
Adenosine for stable SVT requires a 6mg IV bolus initially, escalating to 12mg if ineffective, followed by a saline flush. Vasopressin, an alternative to epinephrine, is administered as a single 40-unit IV dose. Lidocaine, utilized for ventricular arrhythmias, typically starts with 1-1.5mg/kg IV.
The ACLS provider manual PDF stresses dosage adjustments based on patient weight, renal function, and concurrent medications. It also highlights the importance of understanding concentration calculations to ensure accurate drug delivery, minimizing risks and maximizing therapeutic benefits during resuscitation efforts.
Managing Drug Interactions in ACLS
Crucially, the ACLS provider manual PDF emphasizes awareness of potential drug interactions during resuscitation. Beta-blockers can diminish the effectiveness of epinephrine and dopamine, requiring higher doses to achieve desired effects. Calcium channel blockers may exacerbate bradycardia when combined with certain antiarrhythmics.
Patients on digoxin require careful monitoring, as hypokalemia increases the risk of toxicity when administering adenosine. Amiodarone exhibits numerous interactions, notably with warfarin, necessitating vigilant INR checks. Concurrent use of vasopressors and MAO inhibitors can lead to hypertensive crises.
The manual PDF stresses thorough patient history acquisition to identify pre-existing medications. Understanding pharmacokinetic and pharmacodynamic principles is vital for anticipating and mitigating adverse interactions, ensuring optimal patient outcomes during advanced cardiovascular life support interventions.

Special Considerations in ACLS
The ACLS provider manual PDF details adaptations for pediatric, pregnancy, and co-morbidity cases, emphasizing tailored algorithms and drug dosages for specific needs.
ACLS for Pediatric Patients
Pediatric ACLS, as detailed within the provider manual PDF, necessitates crucial adaptations due to physiological differences from adults. The manual emphasizes the importance of utilizing pediatric-specific drug dosages and equipment – airway management tools, defibrillation pads, and medication concentrations must be appropriately sized.
Algorithms for pediatric cardiac arrest differ significantly, prioritizing effective ventilation and early epinephrine administration. The manual provides clear guidance on determining appropriate chest compression depth and rate based on the child’s age and size.
Bradycardia and tachycardia algorithms also require modification, with a greater emphasis on vagal maneuvers and smaller initial doses of antiarrhythmic medications. The ACLS provider manual PDF stresses the need for a systematic approach, recognizing that many pediatric cardiac arrests are secondary to respiratory failure, highlighting the critical role of airway management and oxygenation. Furthermore, it underscores the importance of family-centered care throughout the resuscitation process.
ACLS in Pregnancy
ACLS in pregnancy, as outlined in the provider manual PDF, demands unique considerations due to physiological changes. These include increased blood volume, cardiac output, and oxygen consumption. The manual stresses prioritizing maternal well-being, recognizing that fetal compromise often follows maternal instability.
Specific algorithms address perimortem cesarean delivery, emphasizing rapid intervention to improve maternal and fetal outcomes. The manual details modifications to medication administration, acknowledging potential fetal effects. Epinephrine, for example, should be used cautiously.
Airway management requires careful selection of techniques, avoiding hyperventilation. The ACLS provider manual PDF highlights the importance of left uterine displacement to relieve aortocaval compression and optimize venous return. Continuous fetal monitoring is crucial throughout resuscitation efforts. Furthermore, the manual emphasizes a multidisciplinary approach, involving obstetricians, anesthesiologists, and neonatologists, to ensure comprehensive care for both mother and fetus.

ACLS for Patients with Specific Co-morbidities
The ACLS provider manual PDF details adapting resuscitation strategies for patients with pre-existing conditions. Individuals with heart failure require careful fluid management, avoiding volume overload. Those with chronic obstructive pulmonary disease (COPD) may necessitate adjusted ventilation rates and oxygenation targets, mindful of CO2 retention.
Patients with diabetes can present challenges due to autonomic neuropathy, potentially masking hypoperfusion. The manual emphasizes glucose monitoring and correction during resuscitation. Renal failure impacts drug metabolism and excretion, requiring dosage adjustments.
Furthermore, the manual addresses ACLS in patients with sepsis, highlighting early recognition and source control. It stresses the importance of vasopressors and fluid resuscitation guided by hemodynamic monitoring. The PDF also covers considerations for patients with pre-existing cardiac devices, like pacemakers or ICDs, during defibrillation or cardioversion. A tailored approach, guided by the patient’s specific comorbidities, is paramount for optimal outcomes.
Resources and Updates
Stay current with ACLS guidelines via the AHA website; regular updates to the provider manual PDF ensure best practices in advanced cardiac life support.
AHA Website and ACLS Updates
The American Heart Association (AHA) website serves as the primary hub for the most current ACLS information and resources. Regularly visiting heart.org is crucial for healthcare professionals seeking updates to algorithms, pharmacological guidelines, and overall best practices in advanced cardiovascular life support. The AHA frequently releases revisions to the ACLS Provider Manual, reflecting the latest scientific evidence and advancements in resuscitation techniques.
These updates are often released in response to landmark studies or changes in clinical practice. Staying informed about these changes is paramount for maintaining competency and delivering optimal patient care. The AHA website also provides access to online courses, continuing education materials, and downloadable resources, including errata sheets detailing specific modifications to the provider manual. Furthermore, the AHA offers a platform for tracking changes and understanding the rationale behind them, ensuring a comprehensive understanding of evolving ACLS standards. Accessing these resources is vital for successful recertification and continued professional development.
Continuing Education and Recertification
Maintaining ACLS certification requires ongoing commitment to continuing education. The AHA mandates regular recertification courses to ensure providers remain proficient in the latest guidelines and techniques outlined in the ACLS Provider Manual. These courses typically involve a combination of online modules, skills stations focusing on practical application, and a written examination assessing knowledge retention.

Recertification isn’t merely a formality; it’s a vital process for reinforcing critical skills and addressing updates to algorithms and pharmacological interventions. Numerous accredited institutions and training centers offer AHA-approved ACLS recertification courses. Providers should verify the course’s accreditation before enrolling. Beyond formal recertification, engaging in regular self-study using the provider manual and participating in hospital-based code simulations are excellent ways to maintain competency. Proactive continuing education ensures providers are prepared to respond effectively to cardiac emergencies and deliver the highest quality of care.
Advanced SystemCare and Potential Conflicts
While seemingly unrelated, discussions surrounding software like Advanced SystemCare surfaced within online searches related to the ACLS Provider Manual PDF. Reports indicate potential conflicts when running system optimization tools during critical tasks, such as accessing or studying digital medical resources. Specifically, some users experienced issues with malware removal scans interfering with document access.
It’s crucial for healthcare professionals utilizing digital versions of the ACLS manual to ensure their systems are stable and free from intrusive background processes. Disabling unnecessary software, including potentially conflicting optimization tools, before engaging with vital study materials or during online recertification courses is recommended. Prioritizing system stability safeguards against interruptions and ensures uninterrupted access to the essential information contained within the ACLS Provider Manual PDF, ultimately supporting effective preparation and competency.
